Conventional IVF
We often hear the term IVF or ‘in vitro fertilisation’ used in the context of assisted reproduction, but do we always know exactly what these terms mean?
In 1978, Louise Brown was born in Great Britain. She was the first ‘test-tube baby’, i.e. the first birth by ‘in vitro fertilisation’ or IVF, an event that revolutionised assisted reproduction.
Four years later, France announced its first IVF birth, Amandine, an ‘in vitro fertilisation’ carried out by Dr René Frydman and biologist Jacques Testart.
The idea is simple in itself, but the technique is tricky to perfect. The idea is to carry outside the woman's body (i.e. ‘in vitro’, i.e. in glass, in this case an incubator) what is usually done naturally in the woman's fallopian tubes (i.e. ‘in vivo’): fertilisation leading to the creation of an embryo and then the birth of a baby.
The aim is to bring spermatozoa and oocytes together in a culture medium as close as possible to the one found in a woman's fallopian tube, in order to achieve fertilisation in the same way as during natural sexual intercourse.
IVF treatment involves 3 stages:
Recovery of male and female gametes, oocytes and spermatozoa:
In order to collect several mature oocytes from women, multifollicillary stimulation is carried out, i.e. an injection of hormones to increase egg production. Ovarian activity is put to rest and then the natural cycle (which produces only one mature oocyte) is replaced by an artificial cycle that allows the maturation of 10 to 20 oocytes by daily injection of hormones. This stimulation is closely monitored by ultrasound and blood tests to check the growth of the follicles and avoid hyperstimulation, which is dangerous to health. This stimulation can have side effects such as weight gain, pelvic heaviness, circulation problems and mood disorders.
When the follicles appear sufficiently mature, ovulation is triggered by an injection of chorionic gonadotropins. 36 hours after this injection, the follicles are punctured under local or general anaesthetic. The punctured follicular fluid contains the oocytes that will be used for fertilisation.
On the day of the oocyte retrieval, the sperm is collected by masturbation in the laboratory (although frozen sperm can also be used, for example in the case of sperm donation) after 3 days of abstinence, then ‘cleaned’ to eliminate the seminal fluid and ‘prepared’ by selecting the most fertile spermatozoa. In some cases, sperm may be taken directly from the testicles by puncture or biopsy.
Fertilisation:
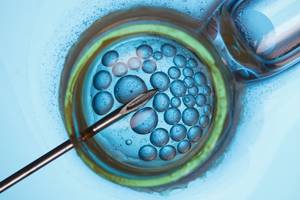
The oocytes collected are then placed individually in containers containing a culture medium favourable to fertilisation and brought into contact with a selection (between 10,000 and 100,000 anyway!) of the ‘best’ spermatozoa (especially the most mobile). These containers are then placed in an incubator at 37 degrees. The number of fertilised oocytes can be seen the next day, and the number of embryos the day after that.
In some cases, sophisticated techniques such as PICSI or ICSI are required to improve fertilisation.
Embryo transfer:
Between 3 and 5 days after fertilisation, the embryos are transferred into the woman's uterine cavity using a fine catheter. If they are transferred at less than 5 days, they are called blastomeres and after 5 days blastocysts (composed of 70 to 100 cells). This implantation at D+5 enables pre-implantation diagnosis to be carried out on the embryos to detect any genetic diseases. Implantation is completely painless. The trend is to implant only one or two embryos to avoid multiple pregnancies and their complications. Of course, it is the medical team that chooses with the couple, but the choice is mainly dictated by the woman's age, the number of previous IVF attempts and certain clinical data.
Supernumerary embryos are vitrified for one or more subsequent attempts.
A pregnancy test is carried out 15 days after implantation.
When is IVF used?
IVF is performed in many cases of infertility, often after unsuccessful attempts at insemination.
Some of the reasons for IVF include endometriosis, changes to the fallopian tubes, after-effects of surgery, impact of some medications, certain types of male infertility or infertility of unknown origin, abnormal cervical mucus, etc.
Causes of failure:
Not all IVF attempts are successful. There are many causes for failure: insufficient or excessive ovarian response to stimulation, failure by the patient to follow the protocol correctly or accurately, absence of oocytes at puncture, poor quality oocytes, cell division arrest, poor quality sperm, poor or non-implantation of the embryo in the uterus.
IVF success rates:
More than 55,000 egg retrievals are carried out each year in the UK.
In 2019, the percentage of IVF treatments that resulted in a live birth was:
- 32% for women under 35
- 25% for women aged 35 to 37
- 19% for women aged 38 to 39
- 11% for women aged 40 to 42
- 5% for women aged 43 to 44
- 4% for women aged over 44
These figures are for women using their own eggs and their partner’s sperm, using the per embryo transferred measure.
This rapid decline with age and low success rates explains why many couples are turning to egg donation.
Similarly, after 4 unsuccessful IVF attempts before the age of 40, it is reasonable to turn to oocyte or embryo donation. After the age of 40, statistics show that donation is virtually the only chance of achieving a pregnancy quickly.
The time between two attempts is generally 6 months, but may be shorter or longer depending on the patient's age.